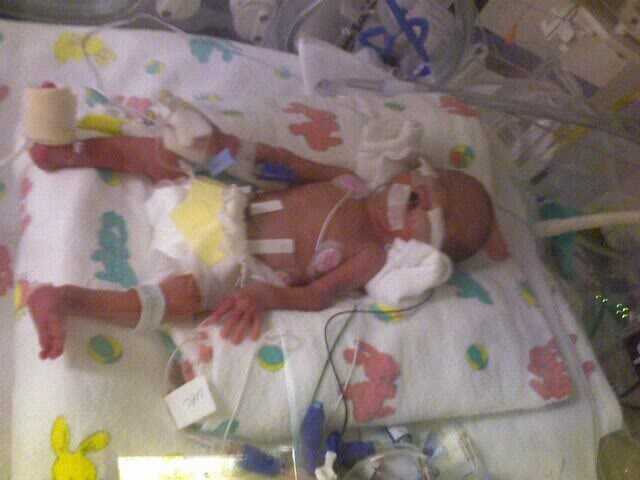
“This cannot be happening AGAIN,” I thought to myself as the labor pains grew more intense. Two years earlier, I had given birth to my first daughter, Hannah, at 27 weeks, 5 days — all 1 lb., 9 oz. of her. And here I was again, 27 weeks, 5 days pregnant and about to give birth to Heaven, my second child.
My second premature child.
As the medical staff worked to stabilize my baby, I could feel a wave of shame and disappointment come over me. Here I was again, having failed to carry my baby full term despite doing all the “right” things throughout my pregnancy. And now this little life would have to endure, fight and struggle to live — away from me and the warmth of my touch. Even worse, it was my fault — or at least that’s what I believed.
While my doctor rushed to keep my baby alive, I began to feel like I was going to die.
“I’m going to pass out… I need help.”
I was shaking violently and struggling to remain conscious, barely able to make my words loud enough to hear. Nurses quickly passed by and reassured me that it was just the pain medication, simply putting blankets on me as they went to get whatever they needed to attend to my baby.
I remember thinking that I didn’t want her to die. That I didn’t want to die. That I wanted her to live… I wanted to live.
But no one seemed to hear me. I mean, really hear me.
What I didn’t know then was that I am the statistic: black women and their newborns are at greater risk of life-threatening birth-related outcomes than white women. In Los Angeles County, black infants die at three times the rate observed for other races before they reach their first birthday. What is more devastating is to know that despite these very challenging starts to my children’s lives, we are considered a success story, for we survived.
It wasn’t until learning these facts at a First 5 LA Board of Commissioners presentation that I realized the shame and self-blame I felt about my birth experience were unwarranted. I felt betrayed by a system that seemingly — from my experience and from established research — was not designed to support me. While this realization was painful, it solidified within me a commitment to be an agent of positive change for children and families. This henceforth inspired me to apply for the 2019 Pritzker Children’s Initiative Fellowship — a competitive national fellowship I was subsequently awarded, as selected by First 5 LA and the Department of Public Health (DPH), the two local organizations chosen to host the fellow.

This Pritzker Fellowship includes full-time funding for two years to work jointly with First 5 LA and DPH to implement elements of the DPH’s Center for Health Equity and Bureau for Health Promotion’s five-year plan to narrow the infant mortality gap. This scope of my work has been helping launch a countywide steering committee dedicated to African American Infant and Maternal Mortality (AAIMM); leading focus groups with the aim of better understanding the African American pregnancy experience, including perceptions of the health care system and racism; and the development of a communications plan to raise awareness of the issue while publicizing solutions and resources to help reduce black maternal stress.
Prevailing assumptions often incorrectly blame these disparities on economic or educational differences between black and white women, or on the varying degrees in the prevalence of risky behavior between the two groups, but emerging research has shown that neither of these are the cause. Notably, college-educated African American mothers nationwide face higher rates of infant mortality, at 5.7 per 1,000 live births, than whites with only high school educations, at 4.2 infant deaths per 1,000. What research does suggest — and what the prevailing narrative fails to show — is that social and psychological stress from lifelong exposure to both structural and interpersonal racism, compounded by implicit bias in the medical field, lies at the heart of black-white birth outcome inequality. In essence, the harmful stress caused by exposure to racism is killing black women and babies through a phenomenon called “weathering” in which such stress acts as a toxic agent in the body.
Through this work, and the 15 focus groups I conducted, I have heard so many stories from other black women that are eerily similar to my own. All of us — at least those who have survived — have carried around pain, guilt and shame until we learn the truth: our bodies are under attack by the world, weathered by the humiliations and injustices of racism, prejudice and bias that we’ve endured daily in both overt and implicit ways. So many of these stories with common themes: “I felt something was wrong, but the doctor didn’t believe me.” “I was treated like I was less than and talked to as if I had no voice in my own pregnancy and birth experience.” Inspired by her own family’s experiences, KPCC Early Childhood Reporter Priska Neely has reported extensively on the topic and shared many of these stories.
Part of my communications strategy as the Fellow has been the development of a website (www.blackinfantsandfamilies.org) dedicated to sharing stories, resources and research — including the conclusions of our focus groups — on AAIMM. Dispelling the untrue narratives and exposing the facts about why African American infants and African American mothers die at disparate rates has been at the heart of this communications strategy. By shining a light on the systemic racism that exists and elevating the voices of those affected, we get one step closer towards identifying and changing the structures that perpetuate the AAIMM crisis.
Another part of my communications strategy has been public presentations and media sponsorships that amplify our findings. Upcoming communications sponsorships include First 5 LA’s sponsorship of the KJLH Women’s Health Expo on May 4th, 2019, which will include radio ads with messaging that will focus on fostering awareness of AAIM, its root causes and what is being done about it; and a table and breakout panel with myself and fellow community leaders discussing “400 Years Is Enough: Ending Black Infant and Maternal Mortality in Los Angeles County.” I will also be presenting our findings at the Center for Health Equity’s Institute of Cultural and Linguistic Inclusion and Responsiveness meeting (internal DPH meeting), and the Countywide Home Visitation Consortium.
Helping launch the African American Infant and Maternal Mortality Steering Committee has been another facet of my work as the Fellow. This committee will lead the county’s five-year Action Plan and determine how to use the recent funds awarded by the California Perinatal Equity Initiative (PEI), as well as ensure readiness for the four-year PEI award that DPH will apply for this summer. We are proud to share that teams in Service Planning Areas 1 (Antelope Valley) and 6/8 (South L.A. and South Bay) — the SPAs with the highest rates of African American infant mortality countywide — have already begun community engagement and local planning activities, including engaging Best Start Communities in those areas. More SPA-level groups are forming, which is so exciting. Participation information can be found here.
This issue is not without hope. In addition to powerful community organizing efforts underway and the bold commitment and investments made by the State of California thanks to the advocacy of Senator Holly Mitchell, First 5 LA and the L.A. County Health Agencies, hope lies in programs and supports that are helping to reduce the pathways of stress for black women, regardless of their income. Implicit bias and anti-racism training for health care providers and county workers has already begun and will continue to expand if SB 464, an assembly bill currently on the floor as introduced by Sen. Holly Mitchell and supported by First 5 LA, is passed, making such training mandatory in all hospitals with perinatal care and alternative birth centers. Increased access to progesterone shots and other clinical interventions, home visitation, doulas and midwives, prenatal and postnatal support groups, policy changes and advocacy are all becoming more widely available — and are all important pieces of the puzzle that are helping to solve this crisis.
In fact, I myself participated in a home visitation program when my children were born. It was a source of support, encouragement and partnership as my husband and I went through the difficult journey of helping our children reach important physical and developmental milestones when they finally came home from the hospital. We also had the support of family members, my church and a great pediatrician who treated us as collaborators in our children’s health and well-being. Today, they are bright, vibrant and strong. They are changemakers in their own right. We are blessed.

Imagine a beautiful ink drawing in every natural hue possible, from pale to ebony, dancing across a canvas… and then just disappearing. That is what it feels like to be in this line of work and to be the subject of it as well.
Black women and our babies are dying at severely disparate rates and many of our babies are entering life way too small and way too early, threatening their development, health and well-being The call to action is for all of us. It is time to rebuild the village for black moms. To look at the disparity not from the lens of the deficit of the mother but from the deficit of our system. I truly believe that change is possible.
Besides, Heaven and Hannah are counting on us.